CTEV and CDH: Causes, Symptoms, Diagnosis, and Treatment
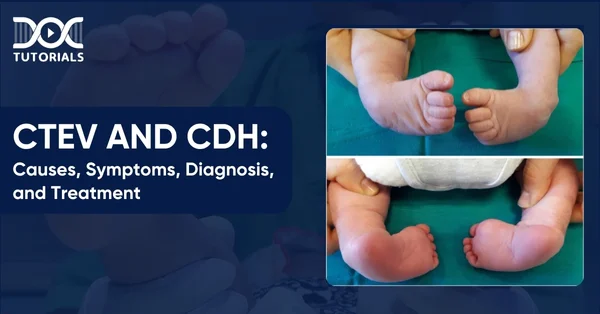
CTEV is a congenital foot deformity, whereas CDH is a severe developmental anomaly where abdominal organs move into the chest through a defect in the diaphragm. Prompt diagnosis and early management of both conditions are crucial to minimise complications and support better long-term outcomes.
For NEET PG aspirants, having an in-depth knowledge of the symptoms, causes, diagnostic procedures, and treatment options for CTEV and CDH is essential. This understanding supports accurate diagnosis and appropriate management, particularly in paediatric and neonatal care.
Keep reading to explore these topics in detail!
What is CTEV?
The CTEV full form is congenital talipes equinovarus. It is commonly known as clubfoot, a condition caused by abnormalities in the tendons — the connective tissues linking muscles to bones. In affected infants, the tendons in the leg and foot are unusually short and tight. This results in the foot being pulled into a twisted position.
Historically, extensive surgical procedures were the primary means of correcting the condition. However, current medical practice generally favours a combination of non-surgical techniques along with a minor procedure to achieve effective and less invasive correction.
What is CDH?
Congenital diaphragmatic hernia (CDH) is a birth defect characterised by an opening in the diaphragm. This defect forms during foetal development and allows abdominal organs to move into the chest area. As a result, the growth and development of the lungs may be severely restricted.
CDH in newborns is considered a life-threatening condition. The last and most serious complication of CDH is its inappropriate lung development that may result in serious breathing problems at birth.
What are the Causes of CTEV?
The following are the causes of congenital talipes equinovarus:
- Genetic Factors
Genes are responsible for guiding the development, structure, and function of the body. An abnormality in one or more genes passed from parents to their children may contribute to the development of CTEV.
- Neurological Conditions
CTEV may develop as a secondary symptom in association with neurological disorders such as spina bifida or cerebral palsy, where muscle imbalance and nerve dysfunction impact foot structure.
- Environmental Influences
Mothers who are exposed to some environmental conditions during pregnancy are at higher risk of producing a baby with clubfoot. These may include the use of harmful substances such as tobacco or drugs, both of which have been associated with a high risk of congenital abnormalities.
- Foetal Positioning in the Womb
Limited space or abnormal positioning in the uterus can restrict foetal movement, which may interfere with normal foot development, contributing to the onset of clubfoot.
What are the Causes of CDH?
In the majority of cases, the underlying cause of CDH remains unknown. Nevertheless, in some instances, CDH has been associated with genetic abnormalities or spontaneous changes in the genes known as mutations.
When CDH is linked to such genetic factors, it may occur alongside additional congenital anomalies, including defects affecting the heart, limbs, eyes, digestive organs such as the stomach and intestines, or other parts of the body.
What are the Risk Factors of CTEV?
Certain factors can increase the likelihood of a baby being born with CTEV foot. These include:
- Gender
Males are approximately twice as likely as females to be affected by CTEV.
- Genetic Predisposition
A history of clubfoot in the family is a great risk factor. When a close relative, such as a parent or sibling, has the condition, then there are higher chances of occurrence in a family member.
- Oligohydramnios
The decreased amount of amniotic fluid that covers and cushions the infant in the mother’s womb may also be a cause of CTEV.
- Environmental Factors
Maternal smoking during pregnancy has been associated with a heightened risk of the baby developing clubfoot.
- Association With Other Congenital Disorders
Clubfoot may be part of broader skeletal abnormalities present at birth. For example, spina bifida is a condition where the spinal cord and spine do not form correctly, which can be linked to an increased risk of CTEV. Similarly, certain chromosomal abnormalities may contribute to the development of this condition.
What are the Risk Factors of CDH?
Multiple risk factors have been associated with the likelihood of experiencing CDH, which are both genetic and environmental. They are listed below:
- Family History
A slight elevation in risk has been observed in individuals with a close family member, such as a parent or sibling, who has been diagnosed with CDH, suggesting a hereditary component.
- Medications and Environmental Exposures
Development of CDH may be caused during pregnancy due to the consumption of some medications and toxic substances. These are as follows:
- Lithium
- Allopurinol
- Mycophenolate mofetil
- Genetic Conditions
CDH may also occur in association with specific chromosomal disorders, including:
- Turner syndrome
- Trisomy 13 (Patau syndrome)
- Trisomy 18 (Edwards syndrome)
- Trisomy 21 (Down syndrome)
What are the Symptoms of CTEV?
CTEV signs are usually observable at birth or in a prenatal ultrasound scan. The common signs of clinical presentation are:
- Unusual Foot Shape
The affected foot tends to be smaller than average; the heel may appear narrower, and the arch may be overly pronounced or missing. These structural irregularities can interfere with proper balance and coordination.
- Abnormal Foot Position
The foot appears twisted or rotated from its normal alignment. In many cases, the sole faces inwards or upwards rather than pointing down. As a result of this deformity, the foot can hardly lie flat on the ground.
- Underdeveloped Calf Muscles
The calf on the affected side is typically smaller and less developed than on the unaffected side. This muscle underdevelopment is usually the result of limited use of the foot and leg during early growth.
- Restricted Movement
Limited flexibility in the foot and ankle is a common characteristic. This rigidity is due to constrained tendons and ligaments that make one find it challenging to position the foot to a normal position.
- Tightened Achilles Tendon
When it is CTEV, the tough tendon that links the heel to the calf muscles, which is called the Achilles tendon, is usually short. This contributes to the downward and inward position of the foot and restricts its natural movement.
What are the Symptoms of CDH?
The signs and severity of CDH newborns can differ based on factors such as the size of the hernia, its underlying cause, and the abdominal organs involved. Common symptoms include:
- Breathing Difficulties
Respiratory distress is often profound. This is mainly caused by compromised lung development in CDH and in acquired diaphragmatic hernia (ADH), due to the compression that the lungs undergo from abdominal organs, which are shifted.
- Bluish Skin Discolouration (Cyanosis)
Inadequate oxygen supply to body tissues may cause a bluish tint to appear on the skin, particularly around the lips and extremities.
- Reduced or Absent Breath Sounds
During clinical examination, there could be silent breathing sounds or the absence of sounds on the affected side of the chest, especially in instances where there has been compromised lung development.
- Presence of Bowel Sounds in the Chest
If parts of the intestines have migrated into the chest cavity, bowel sounds may be audible in the thoracic region during auscultation.
- Rapid Breathing (Tachypnoea)
To compensate for reduced oxygen levels in the bloodstream, the lungs may start to function at an accelerated rate. It results in abnormal, fast breathing.
- Flattened or Less Prominent Abdomen
The abdominal area may appear unusually flat or underfilled, as some abdominal organs may have shifted upward into the chest.
- Increased Heart Rate (Tachycardia)
The heart might pump more, resulting in an increase in heartbeat, in order to supply more oxygenated blood to the body.
How to Diagnose CTEV and CDH?
CTEV and CDH are commonly detected through a prenatal ultrasound scan. It is identified by an imaging technique which produces visual representations of the developing foetus, which allows healthcare professionals to detect structural abnormalities. Diagnosis at an early stage of pregnancy facilitates scheduling of postnatal treatment.
In other instances, the CTEV and CDH condition is diagnosed shortly after birth.
When CDH is suspected, referral to a specialised fetal care centre may be made for a detailed assessment. Additional diagnostic procedures may include:
- Detailed Anatomy Ultrasound
A high-resolution scan is carried out to confirm the presence of CDH and to check for any associated structural abnormalities.
- Fetal Echocardiogram
This specialised form of ultrasound is used to assess the structure and functioning of the developing heart, as congenital heart defects can sometimes occur alongside CDH.
- Fetal MRI (Magnetic Resonance Imaging)
It is a non-invasive imaging procedure that gives additional information on the organs of the foetus, especially when there is ambiguity or incomplete results from the use of ultrasound.
What are the Treatment Options for CTEV?
Commonly used CTEV treatments are as follows:
- Ponseti Method
Regarded as the most effective and widely used treatment for CTEV, the Ponseti technique involves a series of steps:
- Manipulation and Casting: The diagnosed foot is gently repositioned and secured with a plaster cast. This process is repeated weekly for around 6 to 8 weeks.
- Achilles Tenotomy: It is a minor operation done with the aim of relaxing the shortened Achilles tendon, which further allows correction.
- Bracing: After correction, a brace is used to maintain the corrected position and prevent recurrence.
- French Functional Method
This is a non-surgical method that uses stretching exercises, physiotherapy, massage and taping of the foot daily with an aim of realigning it gradually. A trained physiotherapist has to closely oversee the process.
- Physiotherapy
Ongoing physiotherapy plays an important role in improving muscle strength and enhancing flexibility, aiding in the overall function and stability of the foot.
- Orthotic Devices
Orthotic appliances, like braces or splints, are specially worn to help and ensure that the right position of the foot is maintained as the child continues to grow.
- Surgical Correction
In cases where conservative treatment is unsuccessful or when the condition is severe or left untreated, surgery may be necessary. It is usually done through releasing and extending stiff tendons and ligaments, and realigning them.
What are the Treatment Options for CDH?
Managing CDH usually involves a mix of urgent care right after birth and long-term support. A team of experts, including neonatologists, paediatric surgeons, and respiratory therapists, typically works together to care for babies with this condition.
The treatment plan depends on how severe the CDH is and the baby’s general health. It may include:
- Care Before Birth
In serious cases, special procedures like fetoscopic endoluminal tracheal occlusion (FETO) may be done during pregnancy to help the baby’s lungs grow. Doctors often use ultrasound scans and MRIs to closely check the baby’s condition before birth.
- Stabilising the Baby After Birth
Many babies with CDH need help with breathing as soon as they are born. A breathing machine (mechanical ventilator) is often used. In extremely severe cases, the extracorporeal membrane oxygenation (ECMO) procedure can be applied. This machine temporarily takes over the job of the baby’s heart and lungs.
- Surgery
After the baby is stable, surgery is performed to correct a hole in the diaphragm as well as to relocate the organs into their proper position. Even post-surgery, the baby can require breathing assistance. If feeding is difficult, a feeding tube is used.
- Ongoing Care
Long-term follow-up is important, as some babies may have lasting problems such as lung disease or slow development. Respiratory therapy and a proper diet help with recovery. Periodical visits to development professionals can help in monitoring the progress of the baby as it grows.
FAQs About CTEV and CDH
- What is the main cause of CTEV?
CTEV usually results from a combination of genetic, neurological, and environmental factors affecting tendon and muscle development.
- When is CDH usually identified?
CDH is best known to appear during the 16th week of pregnancy, but may appear as early as 10 to 12 weeks and as late as the third trimester. In rare instances, the condition goes unnoticed until after the birth of the baby.
- Can CTEV be permanently corrected?
With appropriate treatment like the Ponseti method, CTEV can be corrected effectively. Nevertheless, consistent follow-up care is essential to maintain the results and prevent the condition from returning.
- Is CDH life-threatening?
Yes, CDH is life-threatening due to underdeveloped lungs and breathing difficulties after birth.
Conclusion
It is imperative to have a good knowledge base about CTEV and CDH and their consequent causes, symptoms, diagnosis, and treatment. Complications can be avoided by early identification and appropriate intervention to enhance the outcome in the affected infants.
Learning in-depth about these topics boosts confidence among NEET PG aspirants to handle complex neonatal problems. DocTutorials is a platform that provides high-yield video lectures, brief notes, and professional guidance to help one get a step closer towards their dream rank. Start your NEET PG preparation with DocTutorials today!
Latest Blogs
-

INI CET Exam 2026: Your Roadmap to Success – Key Topics, Strategies, and Lessons from Last Year’s Papers
The INI CET exam is more than just a test; it’s a significant milestone for many medical students aiming to…
-

INI CET Exam Success: Previous Year Question Papers & Ultimate Guide – INI CET PYQ
One can feel overwhelmed while preparing for the INI CET (Institute of National Importance Combined Entrance Test). A vast syllabus,…
-

NEET PG 2026 Preparation with Live Power Pack: Your Path to Success in 2026
Preparing for the NEET PG 2026 can be an overwhelming journey because of its vast syllabus and the pressure to…