Corneal Ulcer | Causes, Symptoms, Diagnosis, and Treatment
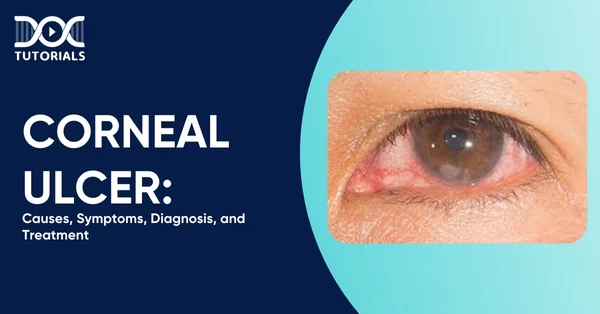
A corneal ulcer is an open sore on the cornea, the transparent anterior surface of the eye. It is a severe ulcer of the eye that most often develops due to bacterial, viral, or fungal infection. It is an emergent medical condition because it may cause irreversible vision damage.
Untreated corneal ulcers can lead to serious complications like lifelong loss of vision or blindness. Recognising corneal ulcer symptoms and understanding their causes and management strategies is vital not just for patient safety but also for NEET PG aspirants like you.
For both medical students and healthcare providers, mastering these topics is essential for academic excellence and effective patient care. Keep reading for an in-depth insight into corneal ulcers.
What are the Causes of Corneal Damage?
Most corneal ulcers are infectious in nature. Here are a few of the common causes:
- Bacterial infections are one of the most frequent causes of corneal damage.
- Infection with viral causes, such as herpes simplex virus (cold sores) or varicella-zoster virus (chickenpox and shingles), can also cause ulcers.
- Fungal infections, though less frequent, can be caused by such pathogens as Fusarium, Aspergillus, or Candida. These are generally seen following eye trauma with vegetable material, i.e., a tree branch.
- Acanthamoeba, a parasite naturally occurring in reservoirs such as soil or freshwater, can also cause severe corneal ulcers, especially among contact lens wearers.
Other causes of corneal damage include:
- Exposure to chemical irritants.
- Foreign material in the eye, like sand or dust.
- Impact by an object, like a tree branch.
- Radiation damage from the sun, sun lamps, welding, or the reflection of the sun off snow (snow blindness).
- Complications of contact lens use.
A corneal erosion can recur if the abrasion re-tears. A corneal infection, also known as keratitis, is relatively uncommon. However, several conditions can lead to a corneal infection, including:
- Conjunctivitis (Pink Eye): Conjunctivitis is an infection caused by a bacteria, virus, or allergen and typically results in minimal irritation of the eye. Yet, if it becomes severe or remains untreated, it can progress to a corneal infection.
- Herpes Zoster (Shingles): This is caused by the same virus that causes chickenpox. In some people, the virus will reappear later in life to produce a painful rash of blisters called shingles. Shingles that appear on the face, head, or neck can also involve the cornea. About 40% to 60% of people with shingles in these areas will have corneal involvement.
- Ocular Herpes: Ocular herpes is caused by the herpes simplex virus, the same virus that causes oral and genital herpes. Ocular herpes occurs on or around the eyelid or eye surface and can result in corneal inflammation.
- Corneal Dystrophies: These are relatively rare illnesses which alter the cornea. There are over 20 known varieties, and these hereditary eye conditions mean that you may be at risk if a relative of yours has one.
Corneal dystrophies usually occur in both eyes and cause blindness and vision loss. Occasionally, they present no symptoms and are only found during a routine eye examination.
What are the Symptoms of a Corneal Ulcer?
You may have signs of infection before you even realise the corneal ulcer is present. Infection signs include:
- Itchy eye
- Watery eye
- Pus-like eye discharge
- Burning or stinging eye
- Red or pink eye
- Sensitivity to light
Signs and symptoms of the corneal ulcer itself include:
- Inflammation of the eye
- Sore eye
- Drooping tears
- Misty vision
- A white spot on your cornea
- Swollen eyelids
- Pus or eye discharge
- Sensitivity to light
- Foreign body sensation
All of the signs of corneal ulcers are serious and need to be treated right away to prevent blindness. A corneal ulcer itself appears as a white or grey spot or patch on the otherwise clear cornea. Some corneal ulcers are too tiny to see without a microscope, but you will experience the symptoms.
How are Corneal Ulcers Diagnosed?
To diagnose a corneal ulcer, an eye doctor or other medical professional will initially depend on an eye test. While a typical check-up reveals everything about the eyes, these tests will be more specific to issues.
One particular laboratory test the provider might conduct is a swab culture. This involves using a soft-tipped swab to collect some discharge from the eye, which is then sent to a lab for testing. The test results can inform the provider about the type of infection causing your ulcer.
In cases that do not respond to initial corneal ulcer treatment, the provider may suggest taking this a step further by performing a corneal biopsy. This procedure involves taking a tissue sample from the cornea for analysis.
Your eye specialist can provide more information about any other tests they recommend. They can also explain how the tests work, their intended benefits, and any expected side effects.
What is the Treatment for Corneal Ulcer?
Listed below are the common treatment options for corneal ulcers:
- Medications
Depending on what caused the ulcer, antibiotic, antiviral, or antifungal eye drops might be given. The patient might need to administer these as frequently as once an hour for several days. For pain, the doctor might also give oral pain medication or drops to dilate the pupil.
- Surgery
If drugs do not work or the ulcer is deep, the patient will need a corneal transplant. This is a procedure where the doctor removes the damaged cornea and inserts a donor’s healthy cornea into the body.
- Treatment Follow-Up
The patient will visit the doctor daily until they tell them to discontinue. Call them right away if symptoms of a corneal ulcer increase, such as increased blurriness of the vision, pain, or discharge.
- Corneal Ulcer Home Treatment
The physician may also recommend what the patient can do at home to feel comfortable:
- Treat the eye with cool compresses, but handle it very carefully so that water does not go into it.
- Avoid touching or rubbing the eye with your fingers.
- Prevent the infection from spreading by washing hands frequently and drying them with a clean towel.
- Take over-the-counter pain medication such as acetaminophen or ibuprofen.
FAQs About Corneal Ulcers
- How long do you wear contacts following a corneal ulcer?
Generally, eye doctors recommend waiting at least two weeks after the ulcer has fully recovered before considering the use of contact lenses again. This timeframe may vary based on individual circumstances.
- Can a corneal ulcer recur?
Viral corneal ulcers (often caused by herpesvirus) can be triggered to recur by physical stress or may reappear spontaneously.
- Do corneal ulcers lead to blindness?
Corneal ulcers are a vision disorder emergency. They need to be treated right away because they can result in permanent eye injury, impaired vision, and even blindness, particularly if not treated with appropriate corneal ulcer care.
- Does corneal damage recover?
Most surface injuries to the cornea typically recover very quickly with treatment, with the eye usually returning to normal within 2 to 3 days. For more severe injuries or instances of delayed recovery, the placement of an amniotic membrane (derived from purified placental tissue) can be highly beneficial.
Conclusion
Corneal ulcers are a critical eye health emergency that, if not promptly treated, can threaten vision. Mild eye trauma can cause ulceration, especially in contact lens users or individuals with a history of eye surface disease. If you notice redness of the eyes, pain, blurred vision, or discharge that is not normal, visit an eye care professional urgently.
Corneal ulcers must be evaluated and treated early to avoid complications. For NEET PG students, in-depth knowledge of such clinical conditions is required, not only syllabus completion but also practice in formulating diagnostic reasoning for the future.
Platforms like DocTutorials are designed to support your learning with concise video lectures, focused quick revision programs (QRPs), and well-structured high-yield notes tailored for both exam success and clinical readiness.
Explore DocTutorials’ NEET PG course today and elevate your preparation.
Latest Blogs
-

NEET SS Exam 2024: Analysis, Key Dates, Counselling
The NEET SS 2024 exam kicked off on March 29, 2025. Over two days and two slots, candidates across 13…
-

NEET PG Registration 2025: An Essential Guide For Exam Prep
The NEET PG registration, which is conducted online, is a crucial step in the exam process. Filling out the NEET…
-

NEET PG Exam 2025- Date, Pattern, Marking Scheme, Subject Wise Weightage, and Exam Mode
NEET PG Exam 2025 is the ultimate gateway for medical graduates aspiring to pursue postgraduate courses in medicine, including MD,…





