Pemphigus: Causes, Symptoms, Diagnosis, and Treatment
In India, a study in the Thrissur district identified a pemphigus incidence of 4.4 cases per million population per year, but its incidence around the world varies widely by region. Therefore, pemphigus has a minor, yet significant share of dermatology outpatients in India.
If you are preparing for the NEET PG examination, then you must learn about pemphigus, including its causes, symptoms, diagnosis, and treatment.
Read on to learn more about pemphigus.
What is Pemphigus?
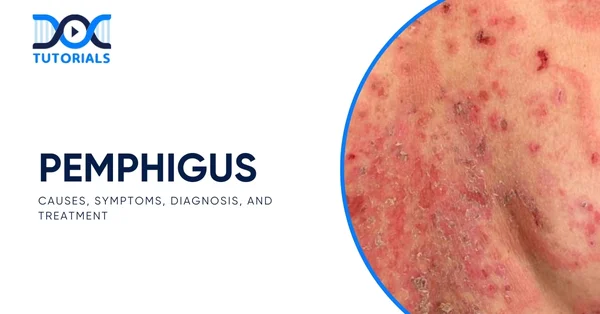
Pemphigus is a rare combination of autoimmune skin diseases that includes transparent blisters and erosions of the skin and mucous membranes in the oral cavity and the genital areas. It is most common among older or middle-aged people.
It is highly important to identify these cases in the initial stage and treat the condition because it appears to respond better to the therapy at an early age. Treatment management usually entails prolonged application of immunosuppressive drugs to control the disease activity and avoid new lesions.
What are the Types of Pemphigus?
Pemphigus can be classified by location and cause of the lesions. The primary ones are the following:
- Pemphigus Vulgaris: It is the most widespread one in the world, including the west. Blisters develop in the mouth and in certain instances, the skin or other mucous membranes. They develop in the superficial layers of skin, are usually painful, and take a long time to heal.
The groin and lower limbs are some of the common sites of skin. The lesions usually take the form of either red or white fluid-filled blisters or open sores.
- Pemphigus Vegetans: A rare form of pemphigus vulgaris consisting of thicker, wart-like lesions tending to be found where the skin folds come in contact, e.g., groin, armpits.
- Drug-Induced Pemphigus: Drug-induced pemphigus may develop either as a side-effect of a few medications, such as some antibiotics and antihypertensives, or as a reaction to a drug. The lesions can develop during weeks or months after the medicine is initiated.
- Pemphigus Erythematosus (Senear-Usher Syndrome): An overlap disorder with Lupus; red scaly crusts on the upper back, chest, cheeks, and the scalp develop.
- Pemphigus Foliaceus: Affects only the top skin layer. Blisters appear on the head, face, neck, and back, but rarely on the mouth. They can be easily torn apart, leaving behind crusty lesions that can extend extensively. The lesions are highly likely to develop in groups, and their colour can vary between red and purple.
- Endemic Pemphigus (Fogo Selvagem): A type of pemphigus foliaceus that is mostly seen in rural parts of South and Central America, especially Brazil.
- Paraneoplastic Pemphigus: The least common type, which happens when there is already a cancerous tumour. It causes severe, persistent mouth blisters, and its diagnosis prompts a thorough search for an associated cancer.
What Causes Pemphigus?
The exact cause of pemphigus is not entirely clear, and the research based upon it shows that genetic predisposition plays a role in the occurrence of the condition, as does the environment.
Pemphigus is an autoimmune disorder, meaning the body’s defence system, the immune system, mistakenly targets healthy skin and mucous membrane cells as if they were harmful invaders. This immune response causes the separation of the linkages of the skin cells, resulting in the production of weak blisters and sore spots, causing pain.
In exceptional cases, pemphigus may be induced using some medicines. These are reported to include penicillin (an antibiotic), piroxicam (an anti-inflammatory non-steroidal medicine used against ailments like rheumatoid arthritis), and antihypertensive medicines.
Also, research found that there is a specific set of HLA (human leukocyte antigen) genes, which are necessary to activate the immune system and are potentially susceptible to specific types of pemphigus.
What are the Symptoms of Pemphigus?
Depending on the type, pemphigus might show differently, but typical symptoms include:
- Blisters
- Redness all over
- Crusted sores
- Bleeding
- Skin that is delicate
- Discomfort or pain
- Itching
Signs of Secondary Infection
Blisters and sores are prone to infection. Possible infection indicators include:
- Pus formation
- Increased pain or burning when touched
- Yellow crust forming after blister rupture
- Delayed healing
- Swelling in the surrounding area
Severe or Systemic Symptoms
In more advanced or severe cases, patients may also experience:
- Fever
- Fatigue
- Vision problems or sensitivity to light (photophobia)
What is the Diagnosis of Pemphigus?
A doctor will confirm a diagnosis of pemphigus through a combination of clinical assessment and investigations:
- Medical History and Physical Examination: A physician will enquire about the symptoms, when they began, and the existence of any co-morbid medical conditions. Then, a physical examination of the skin and mucous membranes will be performed to rule out indications of blistering/erosions.
- Skin Biopsy: To look for distinctive alterations like acantholysis, a tiny sample of the afflicted skin is removed and examined under a microscope.
- Blood Tests: To identify the particular antibodies (autoantibodies) that are causing the illness, a sample of blood is examined.
What are the Treatment Options for Pemphigus?
Depending on the severity, extent, and general health of each patient, treatment for pemphigus is customised. It typically entails a mix of medication, wound care, and careful specialised observation.
General Treatment Measures
- Medication to promote skin healing and reduce the risk of infections.
- Stopping any triggering medicines if they are suspected to have causing symptoms.
- Wound care for blisters and erosions to prevent infection and promote recovery.
Stages of Treatment
Typically, management is done in 3 steps:
- Control Phase: Large doses of medication are given to stop blisters from forming and to start the healing process for blisters that have already formed.
- Consolidation Period: Until most of the blisters have gone away, pharmaceutical use is continued continuously.
- Maintenance Phase: The dose of medication is tapered down to a minimum effective level and then kept as low as possible to discourage the development of new blisters.
Medications Commonly Used
- Corticosteroids: Reduce inflammation and inhibit blister formation. These can be administered orally, intravenously, or topically as creams or ointments.
- Immunosuppressive Agents: Help control the autoimmune attack on healthy skin cells. Examples are azathioprine, mycophenolate mofetil, and cyclophosphamide.
- Rituximab: A monoclonal antibody that targets B cells responsible for producing harmful antibodies.
- Intravenous Immunoglobulin (IVIG): Infusion of healthy antibodies that help neutralise the autoantibodies causing the disease.
- Antibiotics: Used if secondary bacterial infections develop in pemphigus lesions.
FAQs about Pemphigus
- Is pemphigus contagious?
No, pemphigus is not contagious. It is an autoimmune disorder, hence the immune system of the body can destroy its skin and mucous membranes. One is not able to contract it through another person by contact or otherwise.
- Can pemphigus be treated?
Yes, pemphigus can be treated effectively with medications such as corticosteroids, immunosuppressants, rituximab, and supportive wound care. Early diagnosis and prompt treatment improve outcomes and help control symptoms, reducing the risk of serious complications.
- What are the self-care measures to manage pemphigus?
Self-care includes gentle skin cleaning, avoiding trauma or scratching, using prescribed wound dressings, following medication schedules, eating soft foods if mouth sores are present, and promptly reporting new symptoms or signs of infection to your healthcare provider.
- Is pemphigus treatable?
Yes, pemphigus is treatable. While there is no permanent cure, most patients can achieve remission with timely treatment, including corticosteroids, immunosuppressants, and targeted biologics, along with regular follow-up and supportive care to maintain skin health.
- How can I prevent pemphigus?
There is no known way to prevent pemphigus, as it is an autoimmune condition. However, avoiding known drug triggers, seeking early medical attention for skin lesions, and adhering to treatment plans can reduce flare-ups and complications.
Conclusion
Pemphigus should be suspected when a patient presents with persistent flaccid blisters or erosions on the skin and mucous membranes, particularly the oral cavity. Prompt diagnosis and appropriate immunosuppressive therapy are essential to prevent complications and improve long-term outcomes.
If lesions persist, spread, or show signs of infection, urgent dermatological evaluation is vital to confirm the diagnosis, rule out other blistering disorders, and initiate targeted treatment. With expertly curated video lectures, detailed revision notes, and high-yield study material, DocTutorials is a trusted platform for mastering clinical conditions like pemphigus.
Enrol in our NEET PG course today and take the next step towards your medical career!
Latest Blogs
-

INI CET Exam 2026: Your Roadmap to Success – Key Topics, Strategies, and Lessons from Last Year’s Papers
The INI CET exam is more than just a test; it’s a significant milestone for many medical students aiming to…
-

INI CET Exam Success: Previous Year Question Papers & Ultimate Guide – INI CET PYQ
One can feel overwhelmed while preparing for the INI CET (Institute of National Importance Combined Entrance Test). A vast syllabus,…
-

NEET PG 2026 Preparation with Live Power Pack: Your Path to Success in 2026
Preparing for the NEET PG 2026 can be an overwhelming journey because of its vast syllabus and the pressure to…




