Ectropion: Causes, Symptoms, Risk Factors, Diagnosis, Treatment, and Complications
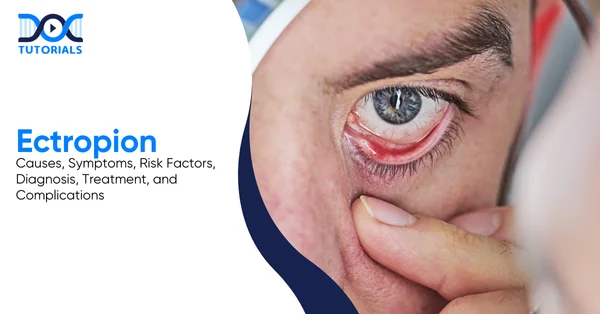
Ectropion could appear as a minor deformity of the eyelids. It is characterised by an outward turning of the eyelids, which can quickly lead to irritation, tearing, and serious complications if the condition goes untreated. Thus, understanding its causes, symptoms, and treatment options is key to preventing long-term damage.
Here’s everything you need to know about ectropion – its risks, diagnosis, treatment, and how it is best managed. Keep reading!
What is Ectropion?
Ectropion is the outward turning of the eyelid, in which the eye is exposed and irritated. The condition may arise from ageing, facial nerve disorders, scarring that pulls on the lid, or something physically weighing on the lid. It helps to know whether it is involutional, paralytic, cicatricial, or mechanical when planning treatment.
Ectropion refers to an eyelid malposition in which the eyelid, usually the lower one, turns outward, away from the eyeball. As a result of its rolled-out nature, the inner surface of the eyelid becomes visible and gives an easily recognisable reddish appearance on examination.
This turning out means that the eyelid does not lie against the eye in a normal manner. Therefore, poor tear drainage and improper protection and lubrication of the eye’s surface occur. This leads to tearing, dryness, irritation, and sometimes inflammation in patients.
Ectropion can affect one or both eyes. It can also involve the upper lid, though that’s less common. This condition is the opposite of entropion, wherein the eyelid rolls inward.
Because the key symptom is exposed conjunctiva, ectropion is easily detected, aiding in the prevention of complications. Artificial tears are the most common starting point for treatment, although chronic cases may necessitate surgery.
What are the Types of Ectropion?
Ectropion can be either congenital, which is rare and present at birth, or acquired. Most of the cases you will encounter are acquired, and they fall into four main types:
- Involutional: This is the most common type, and it occurs due to loosening of the eyelid muscles and ligaments with age, thus turning the lid outward.
- Paralytic: This type develops when the facial nerve isn’t working properly. With the loss of tone of the eyelid, it cannot maintain its normal position and rolls outward.
- Cicatricial: This involves scar tissue. Injury, surgery, burns, or even chronic sun exposure can cause skin contraction, which pulls the eyelid outward.
- Mechanical: This is a case when something physically weighs over the eyelid, such as a tumour or mass, and this lid gets displaced, turning outward.
What are the Causes of Ectropion?
Ectropion is generally caused by age-related loosening of the muscles and ligaments of the eyelid, but may also be caused by facial nerve palsy, scarring of the skin from injuries or surgery, mechanical forces from masses or swelling, and some congenital conditions such as Down syndrome. Additional contributing causes may include stroke, skin cancer, radiation, or rapid weight loss, which can impair the function of eyelid support or nerves.
The causes of ectropion will depend on the type, but most of them boil down to changes in the supporting structures of the eyelid. As tissues naturally loosen with age, muscle weakness and ligament laxity remain the most common reasons people develop ectropion. However, there are several other triggers, too.
The causes of ectropion, based on its type, are given below:
- Involutional Ectropion
In this type of ectropion, the cause is primarily age-related. Over time, the muscles and ligaments lose tone within the eyelids, so the lid is not able to pull tightly against the eye. Chronic eye rubbing can also exacerbate it.
- Paralytic Ectropion
This is because of the malfunctioning of the facial nerve, as in Bell’s palsy and other palsies of the facial nerves. The eyelid tone is controlled by the nerve, and due to its paralysis, the lid droops and rolls outward.
- Cicatricial Ectropion
Scarring pulls the eyelid outward. This can occur after blepharoplasty, trauma, burn injuries, chemical injuries, and even chronic sun exposure. Any contracted scar tissue may pull the lid away from the eyeball.
- Mechanical Ectropion
Here, something physically weighs the lower eyelid down, such as a tumour, mass of the eyelid, fat prolapse, or considerable oedema. Because it is weighted down, the lid cannot remain in its usual position.
- Congenital Ectropion
This is present at birth. Conditions such as Down syndrome or blepharophimosis syndrome increase the chance of an outward-turning eyelid.
- Other Contributing Factors
Some individuals have ectropion due to the following:
- Stroke
- Eyelid skin cancer
- Radiation
- Rapid weight loss
- Previous eye surgeries
In general, the aetiology usually points either to tissue laxity, nerve dysfunction, scarring, or mechanical pull. Identification of its cause does matter, since the treatment approach generally relies on what is actually driving the malposition.
What are the Risk Factors of Ectropion?
Anything that weakens, loosens, or pulls on the eyelid makes ectropion more likely. The biggest risk is age, but it can also be due to past eyelid surgery, injuries, chronic sun exposure, rubbing the eyes, and certain skin conditions. Facial nerve palsy and long-term use of some eye drops may also weaken the support to the eyelids. Anything that affects eyelid tone or skin elasticity thus increases the risk for ectropion.
There are several factors that will increase the likelihood of ectropion development. The key risk factors include:
- Ageing: With a laxity of the eyelid muscles and ligaments taking place over time.
- Previous Surgery on the Eyelid: Procedures such as blepharoplasty can alter the support and increase the risk.
- Eyelid Injuries or Trauma: Cuts, burns, and other types of damage can weaken the lid or distort its shape.
- Chronic Sun Exposure: This leads to long-term UV damage, affecting skin elasticity.
- Frequent Eyelid Rubbing or Pulling: This can stretch the tissues, so the lid cannot stay in place.
- Wearing Contact Lenses: If contact lens insertion/removal habits pull on the lid, it increases the risk of developing ectropion.
- Skin Disorders: Skin disorders of the eyelids, including dermatitis or chronic inflammation.
- Facial Nerve Palsy or Facial Paralysis: This is a condition due to the eyelid losing its tone and drooping.
- Prolonged Use of Some Eye Drops: Certain formulas of eye drops can irritate or weaken eyelid tissues.
Generally speaking, anything that loosens, injures, or tugs on the structures of the eyelid can put one at risk for ectropion.
What are the Symptoms of Ectropion?
Ectropion results in irritation, dryness, redness, and, at times, persistent watering of the eyes. The individual may experience foreign body sensation, crusting, or discharge, or even develop recurring conjunctivitis. If there is a sudden pain, hypersensitivity to light, or dimming of vision, urgent medical attention is required.
Because ectropion involves an eyelid which either poorly protects or lubricates the eye, symptoms often do not take very long to appear. The outward turning of the lower lid can cause the tears not to drain correctly and to leave the eye exposed longer than it should.
This results in dryness mixed with irritation and excessive tearing, symptoms which sound contradictory but happen all the time in ectropion.
Common symptoms include:
- Foreign body sensation, like there’s sand, grit, or something stuck in the eye.
- Dryness because the tears are not evenly spread on the surface.
- Redness is attributed to both irritation and exposure of the conjunctiva.
- Burning or stinging that may worsen during the course of the day.
- Excessive tearing, due to puncta being unable to drain the tears when the lid is pulled outward.
- Light sensitivity from surface dryness and inflammation.
- Watery or mucous-like discharge, especially upon waking.
- Crusting of the eyelashes, which results from the accumulation of secretions during the night.
- Chronic conjunctivitis, recurrent “pink eye” due to constant exposure.
Symptoms that require immediate professional medical intervention include:
- Suddenly, severe sensitivity to light
- Rapidly increasing redness
- Diminished or cloudy vision
These could indicate complications or worsening ocular surface damage and must not be disregarded.
What is the Procedure of Diagnosis for Ectropion?
Diagnosis of ectropion is essentially clinical, and the outwardly turned eyelid is usually pretty obvious. The lid position, laxity, and speed of snap back are examined, as well as the cornea for dryness or damage. The physician will also examine for scars, skin changes, or masses and review medical history to identify the exact cause of ectropion. These steps allow a doctor to choose the appropriate treatment and avoid complications.
The diagnosis of ectropion is mostly clinical, and it does not take that long for a medical professional to notice it. Since the lower eyelid normally sits about 1-2 mm above the inferior corneal limbus, any drooping or outward turning becomes fairly apparent rather quickly. But a proper diagnosis still involves a structured exam, because the cause and severity matter for treatment.
Here’s how the evaluation usually goes:
| Diagnostic Procedures | What It Involves | Why It’s Done |
| Clinical Examination | The doctor inspects the eyelid position, lid laxity, lid margin, and whether the eyelid pulls away during blinking. | Helps confirm that the lid isn’t sitting properly and rules out entropion or other eyelid malpositions. |
| Snap-Back Test | The lower eyelid is gently pulled downward and released. | If the lid doesn’t “snap back”, it indicates poor tone or laxity. |
| Distraction Test | The lid is pulled forward horizontally. | Measures horizontal laxity and determines whether surgery is needed. |
| Slit-Lamp Examination | Evaluates the cornea, conjunctiva, and tear film. | Checks for exposure keratopathy, dryness, irritation, or corneal damage. |
| Facial Nerve Assessment | Look for signs of facial palsy—like incomplete eye closure or weak facial muscles. | Identifies paralytic ectropion, since nerve dysfunction can worsen eyelid drooping. |
| Imaging (if required) | CT or MRI only when tumours, trauma, or scarring are suspected. | Helps rule out structural causes like fractures or mass lesions. |
| Tear Function Tests | Schirmer test or tear breakup time (TBUT). | Assesses how much dry-eye–related damage has occurred due to eyelid eversion. |
What are the Treatment Options for Ectropion?
Ectropion treatment involves eye protection, accomplished with the use of lubricating drops, gels, and ointments, but most cases will eventually require surgery. Depending on the cause, doctors may tighten the eyelid with a lateral tarsal strip procedure or use skin grafts when scarring pulls the lid down. Scar management, stopping harmful eye drops, and treating skin conditions may also help.
The treatment options for ectropion are explained below:
- Lubrication & Ocular Surface Protection
Treatment almost always begins with aggressive lubrication: artificial tears, gels, and ointments. These protect the cornea so it doesn’t dry out or get damaged.
If the ocular surface is stable, there is usually no urgent need to fix the eyelid immediately. However, in cases such as facial palsy, where the cornea is already compromised, the eye can quickly deteriorate. Severe exposure may lead to keratopathy, scarring, and even permanent vision loss; thus, early intervention is critical.
Patients may also use skin tape that temporarily lifts the lid, but it has to be done correctly – always under medical guidance. Improper use can worsen symptoms.
- Eradication of Predisposing Factors
Sometimes, ectropion is related to long-term use of certain eye drops. In that case, your provider will have you stop using them.
Similarly, if a skin condition is pulling the lid outward, anti-inflammatory treatment, most of the time steroids, can help stabilise it.
- Non-Surgical Scar Management
In cicatricial ectropion due to scarring or previous lower-lid surgery, stretching of the scar tissue may be helpful.
This can include:
- Steroid injections
- Scar massage
- Softening the tissue over time
However, these methods don’t always work, and many patients still require surgical correction.
- Surgical Treatment (Definitive Management)
Involutional, paralytic, or cicatricial causes of ectropion are usually corrected with surgery. Surgery is usually performed with the use of local anaesthesia and is very effective.
The types include:
- Lateral Tarsal Strip Procedure, Commonly for Involutional Ectropion
This is the standard surgery when there is an issue with eyelid laxity.
It typically includes:
- Lateral canthotomy combined with lower cantholysis
- Complete disinsertion of the canthus
- Removing a small wedge of the lateral lower eyelid
- Reattachment of the lid to the periosteum of the lateral orbital rim
With this, by tightening and repositioning the eyelid, the lid sits properly again, protecting the globe. This procedure is also useful in facial palsy where orbicularis function is poor.
- Skin Grafting For Cicatricial Ectropion
If the skin of the eyelid is vertically shortened, like following an overly aggressive blepharoplasty, trauma, or chronic inflammatory skin disease, a full-thickness skin graft may be necessary.
Common donor sites include:
- Upper eyelid (ipsilateral or contralateral)
- Preauricular skin
- Postauricular skin
Most surgeons find that a skin graft combined with a lateral tarsal strip provides the best result.
In cases when scars are pulling down the eyelid, the surgeon may have to dissect and release the cicatrix. At times, a temporary tarsorrhaphy, including Frost sutures, may be performed in order to support healing and provide for elevation of the eyelid while recovering.
- Multiple Surgeries
Patients with facial paralysis or extensive scarring often require several procedures to re-establish normal eyelid position. Bilateral involvement is not rare, and even if both lids are asymmetrically involved, surgeons may repair both for a more symmetric result.
5. Cuidado Postoperatorio
After surgery, patients may require:
- A temporary eye patch
- Steroid ointment or antibiotic drops
- Cold compresses
- Over-the-counter pain relievers
Most patients don’t have recurring symptoms once healing’s complete.
What are the Complications of Ectropion?
If ectropion is left untreated, the chronically exposed eye may become dry and irritated, susceptible to the development of infections. Over time, this may lead to complications such as conjunctivitis, scratches on the cornea, and even vision-threatening ulcers. Many early complications are minor, but irreversible scarring or permanent loss of vision can result from long-term disease.
If ectropion is not treated in time, the continued exposure of the eye may start giving rise to serious problems. This is because the eyelid is not in the correct position against the eye; thus, the cornea and conjunctiva remain unprotected. The first result of this situation is irritation, but the complications can be much more grave later on.
Here’s what can happen:
- Chronic Irritation and Dryness: The eye’s exposed condition makes it a constant source of discomfort and inflammation.
- Recurrent Conjunctivitis: The fact that the protective barrier isn’t doing its job makes it easy for bacteria to sneak in, causing redness, discharge and that nasty morning crust.
- Corneal Abrasions: The dry, exposed surface can be scratched easily.
- Corneal Ulcers: Left untended, the dryness or infection can develop into deep ulcers, which can badly affect your vision.
- Impaired Vision: Long-term irritation or damage to the cornea can reduce clarity.
- Permanent Blindness: Corneal ulcers or infection can, unfortunately, advance to the point of causing permanent blindness, though this is pretty rare.
FAQs about Ectropion
- Can ectropion go away on its own?
No, it rarely heals on its own. Lubricants can help ease the symptoms, but the position of the eyelid will not self-correct. Most moderate-to-severe cases eventually require surgery.
- Is ectropion serious or dangerous?
Not during the earlier stage of the disorder, but it may be serious if not treated on time. Chronic exposure of the eye’s surface can cause irritation, keratitis, ulcers, or even loss of vision. So it’s not harmless in the long run.
- What are the common causes or risk factors of ectropion?
The most common cause is age-related laxity. Other causes include previous eyelid surgery, facial palsy, scar tissue from trauma/burns, skin disorders, and chronic rubbing.
- What symptoms should make you suspect ectropion?
A drooping or outward-turned lower eyelid, tearing, dryness, redness, irritation, discharge or crusting, and sometimes difficulty closing the eye.
- What are the treatment options for ectropion?
Early symptoms are helped by lubricants, but chronic or severe cases usually require surgical correction aimed at tightening or repositioning the eyelid.
Conclusion
Ectropion is more than just a lid that looks “off”. Because the eyelid rolls outward and no longer protects or properly lubricates the eye, there’s a real risk of dryness, constant irritation, tears, and even serious complications like corneal damage, ulcers, or chronic infection if it’s left untreated.
Procedures such as a lateral tarsal strip or skin graft, in the case of scar-related instances, can restore normal eyelid position, protect the cornea, and prevent vision loss. Ectropion is an important topic when preparing for the NEET-PG or similar exams; hence, its types and available treatment options need to be understood.
Looking for sources for your NEET PG prep? DocTutorials simplifies medical exam preparation through systematic teaching and strong learning tools. From expert video lectures to high-yield Q-banks, everything is just where you need it.
Check out our NEET PG courses today!
Latest Blogs
-

INI CET Exam 2026: Your Roadmap to Success – Key Topics, Strategies, and Lessons from Last Year’s Papers
The INI CET exam is more than just a test; it’s a significant milestone for many medical students aiming to…
-

INI CET Exam Success: Previous Year Question Papers & Ultimate Guide – INI CET PYQ
One can feel overwhelmed while preparing for the INI CET (Institute of National Importance Combined Entrance Test). A vast syllabus,…
-

NEET PG 2026 Preparation with Live Power Pack: Your Path to Success in 2026
Preparing for the NEET PG 2026 can be an overwhelming journey because of its vast syllabus and the pressure to…





