Orchitis NEET PG Guide: Causes, Symptoms, Diagnosis & Treatment
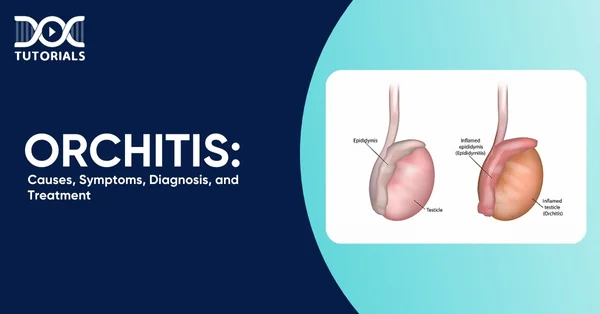
Orchitis is a condition where one or both testicles exhibit swelling, tenderness, and inflammation. It’s typically brought on by infections, including the mumps virus, various sexually transmitted infections (STIs), urinary tract infections (UTIs), or viral infections, such as the mumps virus. For men past puberty, mumps orchitis often leads to intense inflammation.
If not properly treated, orchitis may lead to complications that impact fertility and reproductive function. Identifying the causes and symptoms of this disease is crucial for early diagnosis and effective management.
For those in the healthcare field or aspiring medical professionals, understanding orchitis in depth is an essential step in developing diagnostic expertise and improving patient outcomes.
Interested to learn more? Read on!
What is Orchitis?
Apart from the causes stated above, orchitis is commonly associated with epididymitis, an infection that affects the epididymis. It is the spiral tube found behind the testicle, vital for sperm storage and transport. When both these structures are inflamed, it’s medically termed epididymo-orchitis.
This illness might cause aching and swollen testicles. Orchitis can be relieved with supportive underwear, cold compresses, anti-inflammatory drugs, and antibiotics in some cases. Even with treatment, tenderness of the scrotum might take weeks or months to resolve.
In rare cases, especially in the event of infection during adolescence or childhood, intense orchitis can lead to complications related to fertility (the ability to have children).
What are the Symptoms of Orchitis?
The most prevalent orchitis symptoms include tenderness, swelling, and pain in the testicle. It usually starts in one testicle but often radiates to the other or even to the entire scrotum.
Other symptoms that can be felt with orchitis are:
- Intense fatigue or tiredness
- Signs of infection like fever, headache, and chills
- Red, purple, brown, or black scrotal pigmentation
- General muscle pains
- Nausea and vomiting
- The presence of blood in the urine (haematuria)
- Pain or discomfort during ejaculation (dyscrasia or orgasmalgia)
- Blood found in semen (haematospermia)
- Discharge or leak through the penis
- Rapid heart beating (tachycardia)
What are the Causes of Orchitis?
Orchitis is not typically alone. It tends to be associated with other diseases, particularly infections. Mumps is the most common aetiology, particularly in unvaccinated individuals. In the case of mumps, mumps orchitis typically presents 4 to 6 days following the initial onset of the viral illness.
Other causes may include bacterial infections, such as those originating from urinary tract infections or the prostate gland. These can include bacteria like:
- Staphylococcus
- Streptococcus
- Klebsiella pneumonia
- Escherichia coli
- Pseudomonas aeruginosa
- Viral infections like mumps and rubella that are usually seen in younger individuals
- Other viruses like cytomegalovirus, varicella, echovirus, or coxsackievirus
Bacterial sexually transmitted infections, which include:
- Neisseria gonorrhoeae (gonorrhoea)
- Chlamydia trachomatis (chlamydia)
- Treponema pallidum (syphilis)
Those with impaired immunity can get orchitis caused by less typical pathogens, including:
- Cryptococcus neoformans
- Toxoplasma gondii
- Haemophilus parainfluenzae
- Candida albicans
- Mycobacterium avium complex
How is Orchitis Diagnosed?
The diagnosis of orchitis begins with the doctor’s assessment of the patient’s medical history, followed by a comprehensive physical examination. This is usually done by examining the groin lymph nodes for swelling and examining for swelling of the testicle on the orchitis side.
A rectal exam might also be conducted to look for prostate inflammation or enlargement. Tests and procedures that are commonly included are:
- STI Testing: If there is any discharge from the penis, a small swab can be carefully passed into the head of the penis to get a sample. This is sent to the laboratory to test for infections such as gonorrhoea or chlamydia. Some STI tests can also be carried out using a urine sample.
- Urinalysis: A urine specimen is obtained and analysed in the lab to check for bacterial infection.
- Ultrasound: The imaging tests, especially Doppler ultrasound, are performed to determine the aetiology of the pain in the testicles. This test can help determine whether blood flow to the testicles is reduced, which may indicate torsion. If the blood flow is increased, it supports a diagnosis of orchitis.
What is the Treatment for Orchitis?
Management of orchitis depends on its aetiology. Here is a detailed overview:
Treatment of Bacterial Orchitis
In the bacterial aetiology, antibiotics are given to clear the infection. This is also the case with epididymo-orchitis. With sexually transmitted infection as the aetiology, treatment of the patient’s sexual partner would also be indicated to avoid reinfection.
Patients need to finish the entire course of antibiotics, even if the symptoms resolve before completion of the medication. This will ensure that the infection is eliminated.
Post-treatment, scrotal pain may persist for weeks or months. Home care instructions include rest, wearing an athletic supporter on the scrotum, application of ice packs, and administration of pain medication.
Treatment of Viral Orchitis
In viral orchitis, symptomatic treatment is the course of action instead of virus eradication. The following can be recommended:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) are used, such as ibuprofen (Advil, Motrin IB) or naproxen (Aleve). One needs to see a doctor prior to using this if the patient has kidney disease or is under anticoagulant therapy.
- Bed rest with the scrotum placed above the level of the heart.
- Applying ice packs over the affected area.
Most patients start to feel better within 3 to 10 days. However, complete relief from pain and swelling may take several weeks and, in some cases, several months.
Lifestyle and Home remedies
For patients to have relief from pain and discomfort at home, they can:
- Remain in bed and rest as much as possible
- Lie in a position that raises the scrotum
- Apply cold packs to the scrotum occasionally
- Avoid lifting heavy objects during recovery
FAQs About Orchitis
- Can orchitis cause fever?
In addition to pain and swelling of the scrotum, signs of orchitis may also include fatigue, fever, chills, and headache.
- How long does it take to get orchitis?
Orchitis caused by the mumps virus typically develops a few days after the mumps symptoms begin. Approximately one in three individuals assigned male at birth who contract mumps after puberty will develop orchitis, usually 4 to 7 days following the onset of mumps. Thanks to widespread childhood immunisation, this condition is now less frequent.
- Can orchitis be treated without antibiotics?
Yes, in cases of viral orchitis, orchitis treatment does not involve antibiotics. Instead, patients are advised to manage symptoms using supportive underwear, cold compresses, and anti-inflammatory medications. Nonetheless, recovery can take several weeks or even months, as scrotal tenderness may linger.
- Can orchitis last for months?
While most individuals start to recover from orchitis within 3 to 10 days, it is not uncommon for the pain and swelling to persist. In some instances, discomfort may last for multiple weeks or even a few months.
- Does orchitis require surgery?
Surgical intervention is rarely needed. However, when orchitis leads to complications such as a reactive hydrocele or pyocele, drainage may be necessary to relieve pressure inside the scrotal sac. If there is any suspicion of testicular torsion, an urgent surgical consultation with a urologist is essential.
Conclusion
Orchitis can cause testicular pain and swelling, and emotional reactions like anxiety, discomfort, or frustration. It is perfectly normal to feel anxious when discussing sensitive health information, particularly that of personal body areas. Most people are hesitant to consult with a healthcare provider because they fear being judged or exposed. However, medical professionals are trained to handle such situations with care and understanding, doing their utmost to ensure you feel at ease during examinations and any diagnostic procedures.
For NEET PG candidates, learning about diseases such as orchitis is not merely syllabus work; it’s an integral process towards acquiring the diagnostic acumen required for clinical practice. DocTutorials is dedicated to helping you prepare with video classes by specialists, target-focused Quick Revision Programmes (QRPs), and high-yield notes, all with the aim of making you a champion in competitive exams and your upcoming medical practice.
Check out our NEET PG courses today and navigate your path to medical excellence!
Latest Blogs
-

NEET SS Exam 2024: Analysis, Key Dates, Counselling
The NEET SS 2024 exam kicked off on March 29, 2025. Over two days and two slots, candidates across 13…
-

NEET PG Registration 2025: An Essential Guide For Exam Prep
The NEET PG registration, which is conducted online, is a crucial step in the exam process. Filling out the NEET…
-

NEET PG Exam 2025- Date, Pattern, Marking Scheme, Subject Wise Weightage, and Exam Mode
NEET PG Exam 2025 is the ultimate gateway for medical graduates aspiring to pursue postgraduate courses in medicine, including MD,…