Subarachnoid Haemorrhage: Causes, Symptoms, Diagnosis, and Treatment
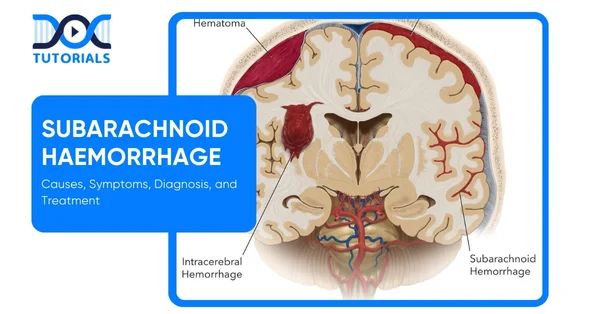
Subarachnoid haemorrhage (SAH) refers to bleeding in the subarachnoid space, which is the space between the brain and the thin protective tissues around it. Subarachnoid haemorrhage is a life-threatening medical emergency where the first sign is a thunderclap headache. Patients always describe this as the worst headache of their lives.
For an aspiring NEET PG student, understanding the symptoms, causes, diagnosis, and treatment of subarachnoid haemorrhage is essential for accurate clinical judgement and effective patient care.
Learn more about subarachnoid haemorrhage in a clear and structured way below.
What is Subarachnoid Haemorrhage?
Subarachnoid haemorrhage (SAH) is a medical emergency due to bleeding between the brain and the tissues that surround and cover the brain. It is a severe medical emergency and always requires prompt intervention. If not treated at the earliest, it can lead to death.
A haemorrhage refers to bleeding or loss of blood from damaged blood vessels. Therefore, subarachnoid haemorrhage refers to excessive bleeding in the subarachnoid space, located just above the pia mater and below the arachnoid mater.
The tissues that cover our brain are called the meninges. The meninges consist of 3 layers and cover the central nervous system, which includes the brain and the spinal cord. These protective membranes are:
- Dura Mater: The outermost tough layer.
- Arachnoid Mater: Located in the middle, it is a web-like membrane that acts as the cushion of the brain.
- Pia Mater: The innermost, delicate layer close to the brain’s surface supplies nutrients and blood.
- Subarachnoid Space: It is not a layer, but refers to the space between the arachnoid and pia mater.
The subarachnoid space is usually filled with cerebrospinal fluid (CSF). Cerebrospinal fluid (CSF) is essential as it plays a role in cushioning the brain from impact and trauma, removing waste products, and providing nutrients. Therefore, not just bleeding but also fluid buildup can have life-threatening consequences.
What are the Causes of Subarachnoid Haemorrhage?
Some of the most common causes of subarachnoid haemorrhage are severe trauma, such as falling from stairs and meeting with a road accident, that severely impact the skull. Another common cause is a brain aneurysm or a ruptured brain aneurysm. In most cases, the exact cause of bleeding is not found.
- Aneurysmal Subarachnoid Haemorrhage
This develops due to the rupture of an intracranial aneurysm, when a bulge in the blood vessel bursts, causing bleeding in the space around it. Common factors that increase the likelihood of this happening are:
- High Blood Pressure: Causes extra stress to the blood vessels
- Smoking: Leads to weakening of the nerves
- Alcohol Use: Dependency on alcohol can raise blood pressure
- Estrogen Deficiency: Lower levels of estrogen are often seen after menopause and can cause inflexibility of blood vessels. Specific factors that are more likely to cause the aneurysm to burst:
- Larger Aneurysm Size: They have thinner walls and hence are more likely to burst
- Age: Blood vessels weaken naturally with age, hence they are more likely to burst
- Circulation Location: Aneurysms in the arteries in the posterior part of the brain are more prone to rupture.
- Atherosclerosis: Fat deposits on the blood vessels make them stiff and fragile.
- Large Aneurysm Size (more than 5 mm): the bigger the aneurysm, the thinner the blood vessel wall, making it more prone to rupture.
- Nonaneurysmal Subarachnoid Haemorrhage (NASAH)
- Perimesencephali Nonaneurysmal Subarachnoid Haemorrhage: A specific pattern of blood is seen in the localised area of the brain, but cerebral angiography (brain scan) is standard. The course of illness is usually benign.
- Occult Aneurysm: It is too small or hidden and is often missed on the first angiography. It is often missed due to its small size, a clot of swelling hiding it, or vasospasm (blood vessels spasm)
- Vascular Malformations: These refer to abnormal connections between the blood vessels of the spinal cord and the brain. It can consist of arteries connecting directly to veins without the normal tiny blood vessels, known as arteriovenous malformations (AVM).
It can also have an abnormal link between arteries and veins, known as a dural arteriovenous fistula.
- Intracranial Arterial Dissection: When there is a tear in the inner wall of a brain artery, bleeding can be massive if the tear spreads through the artery wall.
- Other Causes
- Cocaine Use: Because of the sudden rise in blood pressure, it can lead to subarachnoid haemorrhage (SAH).
- Cerebral Amyloid Angiopathy: A disease usually seen in the elderly, in which amyloid protein deposits in the blood vessels.
- Other Conditions: Sickle cell disease, cerebral venous thrombosis, cerebral vasculitis and bleeding disorders.
What are the Symptoms of Subarachnoid Haemorrhage?
The primary symptom seen in subarachnoid haemorrhage is the thunderclap headache. It is a severe form of headache that quickly reaches high intensity and can last for at least 5 minutes.
Subarachnoid haemorrhage is characterised by certain prodromal events or warning signs that precede the full onset of the condition 10-50% of the time. It usually appears 10-20 days before the actual haemorrhage. The typical early symptoms include:
- Headache
- Dizziness
- Pain around the eye
- Double vision (diplopia)
- Loss of vision
- Numbness, tingling, or weakness in the body.
- Seizures
- Drooping eyelids (ptosis)
- Bruit (hearing a whooshing sound in the head)
- Trouble speaking (dysphasia)
The early signs listed above are often caused by:
- Sentinel Leak: Minor leak of blood that can precede a more serious subarachnoid haemorrhage.
- Mass Effect: Influence or pressure from the mass, like an aneurysm on the surrounding tissues.
- Emboli: Small clots that travel in the blood.
A typical subarachnoid haemorrhage consists of thunderclap headaches. Less severe conditions lead to headaches of moderate intensity, which are followed by neck pain. This headache is accompanied by nausea/vomiting due to meningeal irritation.
When the meninges, the three-layered tissue that covers the brain, become inflamed, they cause nuchal rigidity (neck stiffness), back pain, and bilateral leg pain. Photophobia (intolerance to bright light), focal neurologic deficits, and visual changes are generally common.
During the ictus phase, sudden loss of consciousness (LOC) develops when the patient’s intracranial pressure (ICP) exceeds cerebral perfusion pressure. While loss of consciousness is transient, patients sometimes remain comatose for several days. This depends on where the haemorrhage has occurred and how intense the bleeding is.
How is Subarachnoid Haemorrhage Diagnosed?
Diagnosing a subarachnoid haemorrhage (SAH) is a medical emergency as this is a life-threatening condition, and the earliest intervention can prevent serious complications. It begins with brain imaging, followed by additional tests to determine if the bleeding is minor, older, or not immediately visible.
The table below summarises the key diagnostic steps and their purpose:
| Test | Purpose | Details |
| CT Scan (Computerised Tomography Scan) | First-line imaging | It uses X-rays and computer processing to make detailed brain images, which is best for detecting fresh bleeding. |
| CT Angiography (CTA) | Blood vessel imaging | Contrast dye injected into a vein; shows brain blood vessels to find aneurysms or other vascular causes. |
| Lumbar Puncture | Detects bleeding missed by CT | A needle was inserted in the lower back to collect cerebrospinal fluid (CSF); it was tested for xanthochromia (yellow tint), indicating blood breakdown. |
| MRI (Magnetic Resonance Imaging) | Detects older or small bleeds | Helpful for “subacute” bleeds (a few days to weeks old) not seen clearly on CT. |
| Cerebral Angiogram | Confirms and treats aneurysms | Injects contrast into brain arteries for detailed imaging; often followed by treatment (clipping or coiling). |
What are the Treatment Options for Subarachnoid Haemorrhage?
The management of SAH requires urgent, coordinated care to stabilise the patient, prevent complications, and secure the aneurysm as quickly as possible. Treatment involves a combination of medical therapy, surgical or endovascular intervention, and continuous monitoring, tailored to the severity of the haemorrhage and the patient’s condition.
In treatment, the immediate priority is to secure the aneurysm. This refers to preventing any rebleeding. One of the highest risks in the first 6 hours of a subarachnoid haemorrhage is rebleeding. Endovascular coiling or surgical clipping is used for this. Short-term antifibrinolytics are used if the repair of the aneurysm is delayed.
Blood can block the cerebrospinal fluid pathway, leading to hydrocephalus. Usually, an external ventricular drain (EVD) is placed to relieve pressure and drain cerebrospinal fluid.
Vasospasm and Delayed Cerebral Ischemia (DCI) occur in up to 60% of patients radiographically and 39% symptomatically, caused by arterial narrowing that reduces brain blood flow.
Prevention and treatment of oral nimodipine, maintaining hydration and adequate blood pressure (avoiding hypotension), and, in severe cases, endovascular therapy with angioplasty or intra-arterial vasodilators. The blood pressure is constantly measured to keep it under control.
Electroencephalography (EEG) closely monitors any activity that explains a decline in mental status. Transcranial Doppler (TCD) is used to monitor vasospasm, which detects the blood flow velocity. Monitoring is recommended in patients with large bleeds or low consciousness, and intracranial pressure (ICP).
FAQs about Subarachnoid Haemorrhage
- How long do patients who have subarachnoid haemorrhage (SAH) stay in the hospital?
Your health status determines how long you stay in the hospital. Depending on their state and the requirement for rehabilitation, the majority of patients who experience a subarachnoid haemorrhage are admitted to the hospital for ten to twenty days.
- Is it possible to stop a subarachnoid haemorrhage?
You can reduce the risk by controlling high blood pressure, stopping smoking, reducing alcohol use, and abstaining from recreational drugs like cocaine. Not all instances can be prevented, particularly those caused by genetic or structural vascular anomalies.
Routine health examinations and aneurysm screening are advised for those with a strong family history or known risk factors.
- What is the difference between aneurysmal and non-aneurysmal subarachnoid haemorrhage (SAH)?
When a brain aneurysm bursts, blood leaks into the subarachnoid space, resulting in aneurysmal subarachnoid haemorrhage. This is the most prevalent and severe, frequently necessitating immediate endovascular or surgical treatment.
On the other side, non-aneurysmal subarachnoid haemorrhage can be brought on by trauma, vascular abnormalities, or other circumstances rather than an aneurysm. Its prognosis is often better, but close observation is still necessary.
Conclusion
Early detection and treatment of subarachnoid haemorrhage (SAH), a severe brain emergency, can lessen disability. Understanding the causes, symptoms, investigations, and management is crucial for NEET PG candidates to succeed academically and in clinical settings.
Many patients can regain function and quality of life with prompt intervention and suitable rehabilitation; thus, timely detection is essential to providing successful care.
Take your preparation to the next level with in-depth, exam-focused neurology modules, visual explanations, and high-yield question banks. Learn more by joining DocTutorials and gain access to expert-led lessons, and detailed clinical discussions.
Join DocTutorials and explore our NEET PG course to excel in your medical career.
Latest Blogs
-

NEET SS Exam 2024: Analysis, Key Dates, Counselling
The NEET SS 2024 exam kicked off on March 29, 2025. Over two days and two slots, candidates across 13…
-

NEET PG Registration 2025: An Essential Guide For Exam Prep
The NEET PG registration, which is conducted online, is a crucial step in the exam process. Filling out the NEET…
-

NEET PG Exam 2025- Date, Pattern, Marking Scheme, Subject Wise Weightage, and Exam Mode
NEET PG Exam 2025 is the ultimate gateway for medical graduates aspiring to pursue postgraduate courses in medicine, including MD,…





